Twelve-year clinical trajectories of multimorbidity in a population of older adults
Researchers at Aging Research Center, KI, and collaborators in Italy and Spain, studied how multimorbidity, the occurrence of multiple chronic diseases in the same individual, changed over time in old individuals during a 12-year period using data from the Swedish National study on Aging and Care in Kungsholmen (SNAC-K). The study is published today in the scientific journal Nature Communications.
Multimorbidity is the occurrence of multiple chronic diseases in the same individual, and after 60 between six and nine in ten individuals display this condition. Multimorbidity represents a major barrier for healthy aging, increasing the risk of disability, hospitalization and death. What makes multimorbidity challenging to be addressed in clinical practice is the heterogeneous way chronic diseases combine with each other, leading to very complex disease patterns. The reasons why diseases cluster in the same individuals are different and encompass the sharing of common risk factors and pathological mechanisms (e.g., cigarette smoking), and the fact that they sometimes represent the complications of other diseases (e.g., stroke as a consequence of hypertension). With a joined effort of our group and other researchers from Spain and Italy, we implemented a novel methodology to characterize multimorbidity trajectories over time.
For the first time, in this study we described the natural evolution of multimorbidity over time in individuals aged 60 to 100 years. Using data from the Swedish National Study on Aging and Care in Kungsholmen (SNAC-K), which includes information on more than 3,000 individuals, we identified six different groups of individuals that were sharing the same patterns of diseases: psychiatric and respiratory diseases, heart diseases, respiratory and musculoskeletal diseases, cognitive and sensory impairment, and eye diseases and cancer. The sixth cluster was composed by individuals with less severe multimorbidity, mostly cardiometabolic risk factors (e.g., diabetes and hypertension) that we identified as unspecific multimorbidity. Interestingly, such cluster included 50% of the study population.
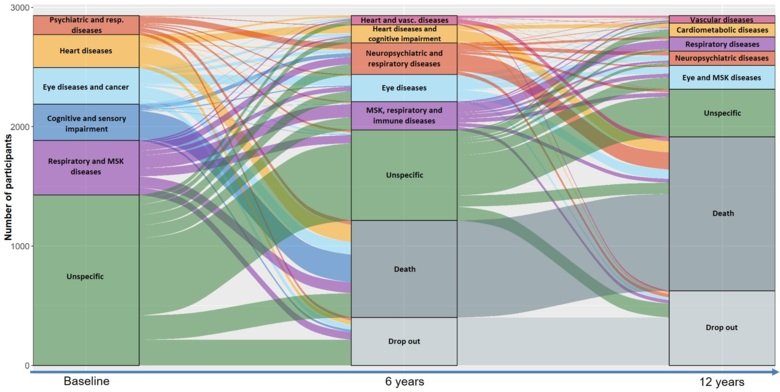
Following the evolution of the multimorbidity clusters over 12 years unrevealed meaningful information for both clinicians and researchers. The first remarkable trajectory involved the group of people part of the unspecific cluster at baseline. The number of participants grouped in this cluster halved during the 12-year follow-up, as the majority transitioned towards other specific multimorbidity clusters identified at follow-ups. Given the young age and less complex clinical picture of these individuals, they may be considered an at-risk population for developing more complex multimorbidity and as such potentially susceptible to preventive interventions. The second relevant clinical trajectory was steered by the high mortality of individuals in clusters characterized by cardiovascular (e.g., heart failure and ischemic heart disease), neuropsychiatric diseases (e.g., dementia and depression) and respiratory (e.g., asthma, bronchitis), which, despite representing only about one fourth of the participants, accounted for more than half deaths during the follow-up period.
Although the ability to discriminate among the potential mechanisms underlying the co-occurrence of multiple chronic diseases needs further improvement, taking into account multimorbidity clusters, and their evolution overtime may enable better decisions for patients with multimorbidity at every health care level and better tailoring of the target population in future intervention studies. The in-depth analysis of the transitions between multimorbidity clusters over time that we have described in our study, will provide unique hints on the mechanisms underlying the complex clinical pictures observed in older people. The person-centred (i.e., clusters of individuals) perspective we have maintained in this study is in line with the principles of personalized medicine, which not only specialist disciplines are approaching, but also geriatric medicine and aging research.
The following researchers were part of the multidisciplinary team working on this project: Davide L Vetrano, Albert Roso-Llorach, Sergio Fernández, Marina Guisado-Clavero, Concepción Violán, Graziano Onder, Laura Fratiglioni, Amaia Calderón-Larrañaga, and Alessandra Marengoni.
Publication
Vetrano, D.L., Roso-Llorach, A., Fernández, S., Guisado-Clavero, M., Violán, C., Onder, G., Fratiglioni, L., Calderón-Larrañaga, A., & Marengona, A. (2020). Twelve-year clinical trajectories of multimorbidity in a population of older adults. Nature Communications 11, 3223. Nature Communications June 26 2020
Grants
This work was supported by the funders of the Swedish National study on Aging and Care (SNAC): the Ministry of Health and Social Affairs, Sweden; the participating County Councils and Municipalities; and the Swedish Research Council. Specific grants were received from The Swedish Research Council for Medicine, the Swedish Research Council for Health, Working life and Welfare (Forte), Gamla Tjänarinnor, and the Ermenegildo Zegna Foundation
