Simple tool shows life expectancy after dementia diagnosis

Researchers at Karolinska Institutet and from the Netherlands have developed a simple tool that shows the survival probability of a person with dementia disease over three years. This, they hope, will facilitate dialogue with the most seriously affected and help doctors and others plan the necessary care. The study is published today in the scientific journal Neurology.
Dementia diseases are currently incurable. There are, however, many kinds of dementia, which develop differently from person to person. Some people can live for many years with their disease, while others have a disease that progresses more aggressively. This means that doctors need a simple tool to indicate the severity of the disease at the point of diagnosis. This can help in planning care and help these patients understand how their disease is likely to develop.
For their study, the researchers monitored patients over the age of 65 who were diagnosed with dementia and registered in the Swedish Dementia Registry between 2007 and 2015. The study included over 50,000 individuals, who were monitored via various health-data registries up to 2016, by which time 20,000 of them had died, on average after a median time of 4.8 years after diagnosis. The researchers examined the effect on post-diagnosis life-expectancy of a number of easily identifiable factors, producing two clear, schematic tables.
Tool for primary care physicians
The first one is for primary care physicians that produces a prognosis based on sex, age, cognitive ability (measured using the MMSE, Mini-Mental State Examination) and comorbidity (measured using the Charlson Comorbidity Index).
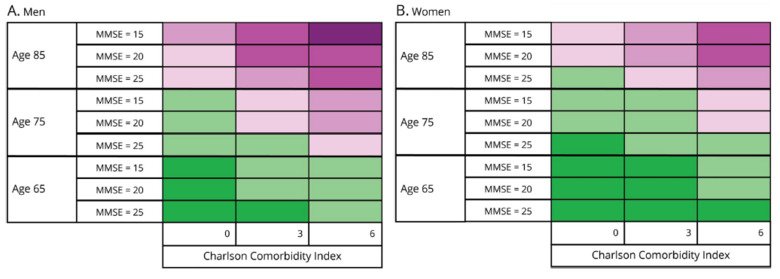
The second table is for specialist clinics, such as memory clinics, that also factors in the specific subtype of dementia (Alzheimer’s disease, for instance, is often less aggressive). Equipped with these parameters, doctors can place an individual case in the schematic table to show how likely it is that the patient will die within three years of diagnosis.
The tool is intended for use by people who care for or treat dementia patients in primary care or at specialist clinics. One aim is to give doctors and care providers a better understanding of which patients are in urgent need of a care plan and who may benefit from additional monitoring. Another goal is to help doctors and other care providers to engage in a dialogue with their patients about their disease and the risk of death.

Useful for conversations on future care
The study’s corresponding author Sara Garcia-Ptacek, a neurologist at Stockholm South General Hospital, says that many patients ask about how their disease will progress, and that a tool like this can be useful to help answer those questions.
“It can also be used in conversations about future care with patients who don’t raise the issue themselves,” says Garcia-Ptacek, who is also a researcher at the Department of Neurobiology, Care Sciences and Society (NVS) at Karolinska Institutet. “In those cases, a tool like this can be an incentive to start such a conversation, which should be held before there are too many cognitive obstacles. This conversation could be about where someone would prefer to live, at home or in other accommodation, or anything else that needs planning.”
The study was conducted with researchers from Radboud University Medical Center in the Netherlands and was financed with grants from the Swedish Research Council, the Swedish Research Council for Health, Working Life and Welfare (Forte), the Swedish Society for Medical Research, the Swedish Order of St John, Region Stockholm (ALF), the Foundation for Geriatric Diseases at Karolinska Institutet, the Loo and Hans Osterman Foundation for Medical Research, Radboud University Medical Center in the Netherlands and Alzheimer Nederland.
Publication: ”Survival time tool to guide care planning in people with dementia”, Miriam L Haaksma, Maria Eriksdotter, Debora Rizzuto, Jeannie-Marie S Leoutsakos, Marcel GM Olde Rikkert, René JF Melis och Sara Garcia-Ptacek, Neurology®, the medical journal of the American Academy of Neurology, online Dec. 16, 2019, doi: 10.1212/WNL.0000000000008745
