New blood test may improve mapping of mosquito-borne viruses
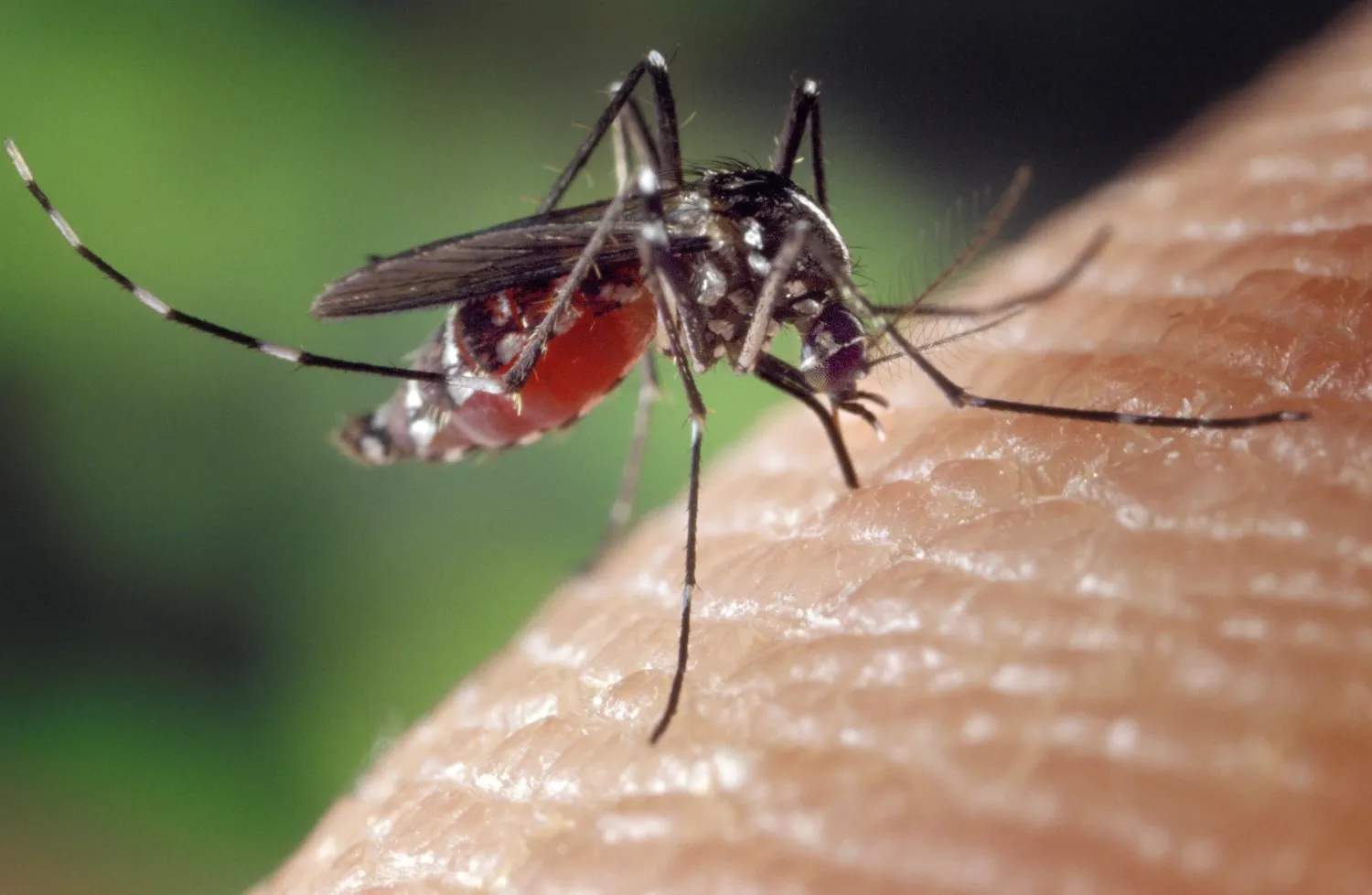
Mosquito-borne viral diseases such as dengue, Zika and chikungunya are spreading to new regions as the climate becomes warmer. A new study from Karolinska Institutet and Institut Pasteur, published in Nature Communications, shows that a newly developed blood test can distinguish between similar viruses and thereby contribute to better surveillance of how these infections spread.

“This type of mapping is crucial for preventing outbreaks and for the effective control and containment of these diseases,” says Victor Yman, infectious disease physician and researcher at the Department of Medicine, Solna, Karolinska Institutet, and the Department of Global Health, Institut Pasteur.
Mosquito‑borne viral diseases constitute a growing global public health threat. As temperatures rise, disease‑spreading Aedes mosquitoes gain wider geographical distribution, increasing the risk of outbreaks even in parts of Europe. To prevent and quickly halt the spread of viruses such as dengue, Zika and chikungunya, more reliable methods are needed to understand how infections move through populations.
Method can distinguish between infections and cross‑reactions
In the present study, researchers at Institut Pasteur in France, Karolinska Institutet in Sweden, and several international partners have developed an antibody‑based method that can distinguish between a true previous infection and cross‑reactions that occur when viruses are closely related.
The researchers analysed just over 4,000 blood samples from Peru, Senegal, French Guiana and New Caledonia. Antibodies against 28 viral proteins from nine different mosquito‑borne viruses — including dengue, Zika, chikungunya and Mayaro — were measured. The aim was to map the spread of different viruses over time in various regions, despite the fact that closely related viruses often generate cross‑reactive antibody responses.
Possible to confirm reaction
To determine which antibody patterns indicate a genuine infection, laboratory tests were combined with mathematical models.
“By combining experimental methods with mathematical models, we can better estimate the extent of transmission of various viruses in an area over time,” says Victor Yman.
A complementary method, in which cross‑reactive antibodies were removed from the samples, also made it possible to confirm whether a reaction was specific to the virus being tested or instead caused by cross‑reactions. This allowed the researchers to see that individuals who initially appeared to have been infected with both chikungunya and the closely related Mayaro virus, in some cases had only been infected with Mayaro but had developed cross‑reactive antibodies that resembled those induced by chikungunya virus infection.
“We see that chikungunya virus more often gives rise to cross‑reactive antibodies than Mayaro virus. This is important to know when interpreting blood test results,” says Victor Yman.
The work is an international collaboration involving researchers in France, Peru, Senegal, French Guiana and New Caledonia. The study was funded by, among others, the Swedish Society for Medical Research, the EU Horizon 2020 programme, the European Research Council, and several international research foundations. The researchers report no conflicts of interest.
Publication
"Investigating antibody cross-reactivity and transmission dynamics of alphaviruses and flaviviruses using a multiplex serological assay", Victor Yman, Jason Rosado, Noé Ochida, Laura Garcia, Marie-Fabrice Gasasira, Gaëlle Baudemont, Estee Cramer, Myrielle Dupont-Rouzeyro, Karl Huet, Maylis Douine, Alice Sanna, Yann Lambert, Gabriel Carrasco-Escobar, Oscar Nolasco, Dionicia Gamboa, Gamou Fall, Oumar Ndiaye, Oumar Faye, Cheikh Loucoubar, Aissatou Toure-Balde, Makhtar Niang, Ines Vigan-Womas, Simon Cauchemez, Michael T White, Nature Communications, online 15 April 2026, doi: 10.1038/s41467-026-71451-7
