Brain imaging can predict Alzheimer’s-related memory loss

Researchers at Karolinska Institutet have imaged tau protein in the brains of living patients with Alzheimer’s disease. The amount and spread of tau proved a predictor of future memory loss. Brain imaging for measuring tau can be useful both for improving diagnosis and for developing more effective treatments, say the researchers. The study is published in the journal Molecular Psychiatry.

Alzheimer’s disease, which is the most common dementia disease, can be caused by accumulations of proteins in the brain that damage the neurons and cause memory loss. However, the disease tends to take an individual course, which makes it hard to predict what symptoms a patient will develop. For around 30 to 50 per cent of patients, their condition can remain stable for many years, especially in the early stages of the disease; for others, deterioration is rapid.
“Modern brain imaging techniques offer new possibilities for predicting how the disease will develop,” says lead author Konstantinos Chiotis, doctor and researcher at the Department of Neurobiology, Care Sciences and Society, Karolinska Institutet. “This is important both as an aid to diagnosis and a means of optimising intervention for the individual patient, and for the development of drugs.”
The KI researchers have previously shown under the supervision of Professor Agneta Nordberg that PET (positron emission tomography) scans can be used to image the distribution of tau protein in the brains of living individuals. Accumulation of tau is linked to Alzheimer’s disease.
Monitored for over four years
In the present study, 20 patients underwent a thorough examination using all existing markers for Alzheimer’s disease at Karolinska University Hospital’s cognitive clinic. They were also given a PET scan to image tau protein in their brains. The researchers then monitored them for over four years so that their cognitive impairment could be assessed over time to find out if the amount of tau could predict the speed of deterioration.
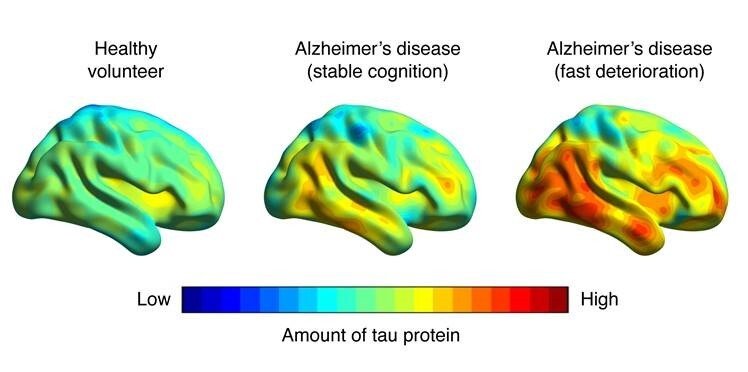
The researchers found that the patients who had low amounts of tau protein initially demonstrated stable function during follow-up, while patients with high amounts of tau protein showed a rapid deterioration in cognitive function. The amount and distribution of tau protein in the brain could differentiate the patient groups with a precision of over 95 per cent, while the precision of the existing clinical markers was at most 77 per cent. The exact amount of tau also tallied well with the exact degree of deterioration on the clinical scale that is routinely used at most clinics as a measure of the cognitive function of patients with memory loss.
May be useful for drug development

“Our results suggest that tau protein has a major influence on cognition,” says Professor Nordberg, who led the study. “This means that drugs targeting accumulations of tau may have a better chance of changing the course of the disease than the treatments that have so far been tested and found wanting.”
The study was financed by the Swedish Foundation for Strategic Research, the Swedish Research Council, Region Stockholm (ALF funding), the Swedish Society for Medical Research, the Loo and Hans Osterman Foundation for Medical Research, the Foundation for Geriatric Diseases at Karolinska Institutet, the Magnus Bergvall Foundation, the Tore Nilson Foundation for Medical Research, the Sigurd and Elsa Golje Memorial Foundation, the Eva and Oscar Ahrén Foundation, the Gamla Tjänarinnor Foundation, the Axel Linder Foundation, the Åhlén Foundation, the Gun and Bertil Stohne Foundation, KI’s funds, the Swedish Brain Fund, the Swedish Alzheimer’s Foundation, Demensfonden (dementia research fund), the Dementia Association and the EU’s INMiND project.
Publication
“[18F]THK5317 imaging as a tool for predicting prospective cognitive decline in Alzheimer’s disease”. Konstantinos Chiotis, Irina Savitcheva, Konstantinos Poulakis, Laure Saint-Aubert, Anders Wall, Gunnar Antoni, Agneta Nordberg. Molecular Psychiatry, online 3 July 2020, doi: 10.1038/s41380-020-0815-4.
