Women severely affected by chronic cluster headache

Cluster headache, sometimes known as “suicide headache”, have been described as a predominantly male disease. New research from Karolinska Institutet now shows that women who have the disease are more affected in their daily lives. They have longer periods of pain, a higher frequency of related symptoms, use more prophylactic medicine and take more sick leave. The results are published in two studies in the journal Neurology, the medical journal of the American Academy of Neurology.

“Cluster headache is still often initially misdiagnosed in women, perhaps because some aspects can be similar to migraine,” says study author Andrea Carmine Belin, associate professor at the Department of Neuroscience, Karolinska Institutet. “It is important for physicians to be aware of how the disorder manifests differently in men and women so the most effective treatment can be given as fast as possible.”
It is about three to five times more common for men to be diagnosed with cluster headache than women. Because the differences were once even greater, the condition has largely been considered a male dominated disease.
The condition affects about one in a thousand people and is characterised by extremely painful bouts of headache that last between 15 minutes and three hours and occur up to eight times a day. The cause of the disease is unknown, but as the attacks tend to follow circadian and annual rhythms, peaking at night and in the autumn and spring, there are speculations that our internal biological clock affects the course of the disease.
Severe variant for women
Researchers at Karolinska Institutet now show that women frequently tend to suffer from the more severe variant of the disease, meaning that they have fewer than three symptom-free months a year – a condition known as chronic cluster headache.
“Men and women report the same level of pain, but since the women’s periods of pain tend to last longer, their daily lives are also more impacted,” Andrea Carmine Belin says.
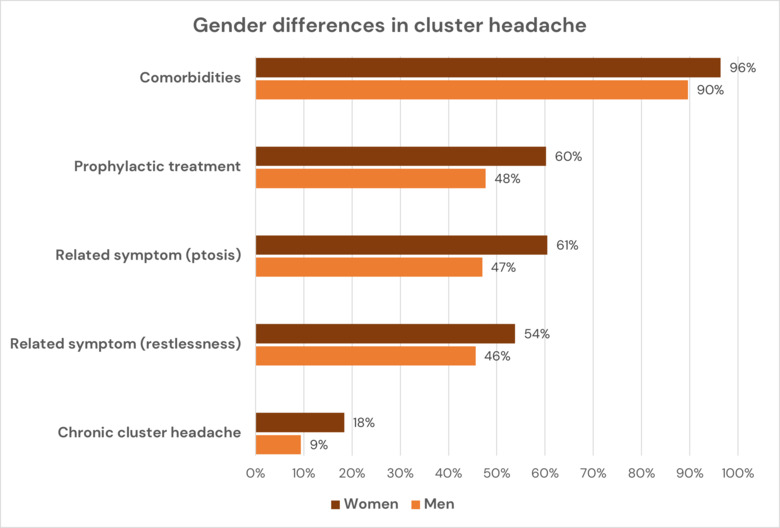
In one of the studies, the researchers found that of the 874 participants, twice as many of the women had the chronic variant of the disease than the men (18 percent versus 9 percent). All participants had been diagnosed with cluster headache by neurologists at clinics in Sweden between 2014 and 2020 and were also asked to complete a detailed questionnaire on lifestyle, symptoms and treatment.
More of the women used prophylactic drugs than the men (60 percent versus 48 percent) and reported a higher frequency of associated symptoms such as drooping eyelids, also known as ptosis (61 percent versus 47 percent), and restlessness (54 percent versus 46 percent). The women had slightly more nightly attacks and more commonly reported sleep deficiencies. It was also twice as common for the women to have a relative with cluster headaches (15 percent versus 7 percent).
“It’s hard to say what’s at the root of these differences, but what we see is that women who are diagnosed with cluster headache tend to present a more severe variant of the disease and that it’s time to stop thinking of cluster headache as a predominantly male disease,” says Caroline Ran, research specialist at the Department of Neuroscience, Karolinska Institutet.
High comorbidity
The other study shows that patients with cluster headache often have other diagnoses, and that here, too, women are over-represented. A full 96 percent of the women amongst the 3,240 patients with cluster headache, resident in Sweden in 2010, had at least one other diagnosis, compared with 90 percent of the men. In a matched control group of 16,200 individuals, multi-morbidity was found in 78 percent of the reference group. The women also took more days of sick leave and were more likely to go into early retirement.

“What’s striking is that almost every woman with cluster headache presents a comorbidity, which reinforces the view that these women suffer severely,” says Christina Sjöstrand, adjunct senior lecturer at the Department of Clinical Neuroscience, Karolinska Institutet. “It’s reasonable to assume that it affects their ability to work and it’s important for the sake of the individual and society that they get help in the form of acute and prophylactic treatment and of follow-up and support.”
The research on cluster headache will continue in part at the newly created Centre for Cluster Headache at Karolinska Institutet, led by the research team of Andrea Carmine Belin.
The study was financed by the Swedish Brain Foundation, the Mellby Gård Foundation, the Swedish Research Council, Region Stockholm, Karolinska Institutet’s research funds and Märta Lundkvist stiftelse. The researchers report no conflicts of interest.
Publications
“Sex differences in clinical features, treatment, and lifestyle factors in patients with cluster headache.” Carmen Fourier, Caroline Ran, Anna Steinberg, Christina Sjöstrand, Elisabet Waldenlind, Andrea Carmine Belin, Neurology, online Dec. 21, 2022, doi: 10.1212/WNL.0000000000201688
“Multimorbidity and sickness absence/disability pension in cluster headache patients and matched references; a Swedish register-based study.” Caroline Ran, Kristina Alexanderson, Andrea Carmine Belin, Gino Almondo, Anna Steinberg, Christina Sjöstrand, Neurology, online Dec. 14, 2022, doi: 10.1212/WNL.0000000000201685
Editorial: "Cluster Headache: Worse in Women." Mark J. Burish, Richard B. Lipton, Neurology, online Dec. 21, 2022, doi: 10.1212/WNL.0000000000206807
