Mini-kidneys help understand the link between diabetes and severe COVID-19
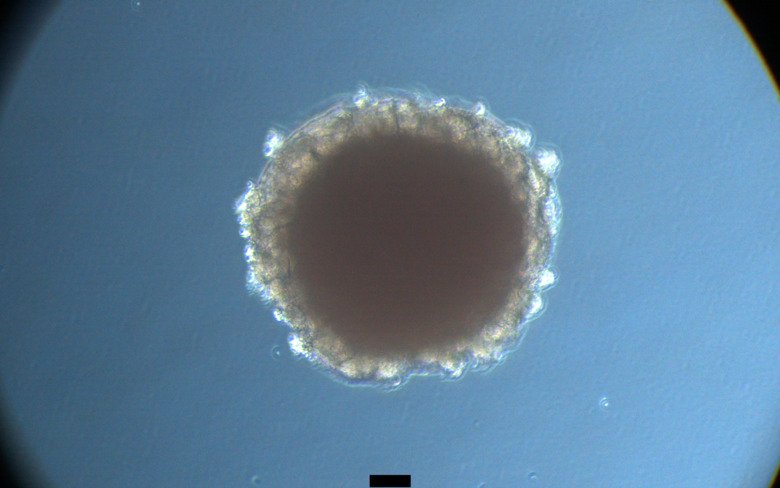
A team of scientists including at Karolinska Institutet has used mini-kidneys simulating those of diabetic patients to further our understanding of the link between diabetes and COVID-19. The researchers found that diabetic mini-kidneys have a higher susceptibility to SARS-CoV-2 infection than non-diabetic mini-kidneys. The study, which is published in the journal Cell Metabolism, also identified genetic evidence for the essential role of the ACE2 receptor in COVID-19.

“This finding sheds light on a potential mechanism behind more severe cases of COVID-19 in diabetic patients. This technology will improve our capability to investigate how viruses interact with different organs in the human body,” says Ali Mirazimi, adjunct professor at the Department of Laboratory Medicine, Karolinska Institutet, and one of the study’s corresponding authors.
Various studies indicate that people with diabetes are more likely to develop severe COVID-19, and that a number of patients hospitalized with COVID-19 suffer acute kidney damage. To date, the molecular and metabolic mechanisms underlying these elements are not fully understood.
In the current study, a team of researchers led by Professor Nuria Montserrat at the Institute of Bioengineering of Catalonia (IBEC) in Spain and involving others from Karolinska Institutet, the University of Florida in the U.S. and the Life Sciences Institute of the University of British Columbia in Canada developed kidney organoids (mini-kidneys) that simulate human conditions in the early stages of diabetes.
Using different molecular biology techniques including gene editing, the researchers observed that in diabetic mini-kidneys it is the abundance of the ACE2 receptor, described as a gateway for SARS-CoV-2 viral entry, that determines susceptibility to viral infection.
Diabetic kidneys more prone to infection
“Our diabetic renal organoid model has allowed us to observe that diabetic mini-kidneys, with a greater number of ACE2 receptors, have a greater susceptibility to viral infection,” says Elena Garreta from the Institute for Bioengineering of Catalonia and first co-author of the study in a press release from IBEC.
Laboratory comparisons of kidney cells from patients with diabetes and individuals without the disease further demonstrated that kidney cells from diabetic patients had more ACE2 receptors and suffered a higher rate of SARS-CoV-2 infection.
“The development of a diabetic kidney organoid is a great step towards experimentally dissecting how metabolic changes can impact SARS-CoV-2 infections. The data again demonstrate that ACE2 is the essential receptor for SARS-CoV-2 even under conditions of comorbidity,” says co-corresponding author Josef Penninger from the Institute of Molecular Biotechnology of the Austrian Academy of Sciences (IMBA) and the University of British Columbia.
To delve into the mechanisms that may explain such observations, the researchers used a compound of substances that modulates the metabolic state of cells and found that the treatment reduced viral infection.
"We have shown that the SARS-CoV-2 virus is capable of directly infecting proximal tubule cells isolated from the human kidney and that diabetes makes these cells more prone to infection," says Megan Stanifer at the University of Florida and first co-author of the study.
This research was supported in part by the Swedish Research Council, the European Research Council, the Institute of Health Carlos III and the Foundation Banco Bilbao Vizcaya, among others.
The authors have declared that a patent has been submitted to use human organoids to study SARS-CoV-2 infections and possibly develop new therapies. Josef Penninger is shareholder of Apeiron Biologics that is developing soluble ACE2 for COVID-19 therapy.
This news article is based on a longer press release from the Institute of Bioengineering of Catalonia (IBEC).
Publication
“A diabetic milieu increases ACE2 expression and cellular susceptibility to SARS-CoV-2 infections in human kidney organoids and patient cells,” Elena Garreta, Patricia Prado, Megan Stanifer, Vanessa Monteil, Andrés Marco, Asier Ullate-Agote, Daniel Moya-Rull, Amaia Vilas-Zornoza, Carolina Tarantino, Juan Pablo Romero, Gustav Jonsson, Roger Oria, Alexandra Leopoldi, Astrid Hagelkruys, Maria Gallo, Federico González, Pere Domingo-Pedrol, Aleix Gavaldà, Carmen Hurtado del Pozo, Omar Hasan Ali, Pedro Ventura-Aguiar, Josep María Campistol, Felipe Prosper, Ali Mirazimi, Steeve Boulant, Josef M. Penninger, Nuria Montserrat. Cell Metabolism, online 12 maj, 2022, doi: 10.1016/j.cmet.2022.04.009
